A Problem of Excess
Epidemics and pandemics are, by definition, fast-moving and difficult to track. These are the diseases that we couldn't keep a lid on, outbreaks that breached our initial efforts at control. It follows then, that ongoing reporting of such diseases won't be entirely accurate, subject to various limitations imposed by testing and recording protocols. This reality is misused by some who believe that reported impacts are exaggerated and societal responses unjustified, but such a belief runs counter to the evidence. Excess mortality is implacable that way; a sufficient number of unattributed deaths will demand explanation eventually, and even the briefest examination of excess mortality figures during the COVID-19 pandemic suggests exaggeration has not been our main problem.
Of course, there have been signs of under-reported mortality since the earliest days of this outbreak, but we'll cite only one example here. Our knowledge of COVID-19's many potential harms has been hard-earned in the most visceral way, both by victims and by healthcare workers on the front-line. In April 2020, the BBC ran a diary entry from a single multi-fatality shift undertaken by New York paramedic Anthony Almojera. The BBC concluded their report with this:
"Not one of the 12 people suspected to have died of Covid-19 on Anthony's shift had been tested for coronavirus. As a result, their deaths were not included in the official coronavirus death toll in New York [...]"
In Seattle, research to better quantify COVID-19 mortality was undertaken by the Institute for Health Metrics and Evaluation (IHME) at the University of Washington School of Medicine. The team studied global mortality over the course of the pandemic and concluded that the true COVID-19 mortality level is more than double that officially reported. Their modelling creates a COVID-19-specific measure of excess mortality over the pandemic period. It does this by accounting both for non-COVID-19 deaths (such as those related to lockdown restricting access to necessary healthcare), as well as pandemic-imposed reduced mortality (such as fewer traffic deaths due to more home working). Figure 1 charts their findings for a range of countries.
Figure 1.Reported and unreported COVID-19 mortality for a range of countries. Data Source: IHME.
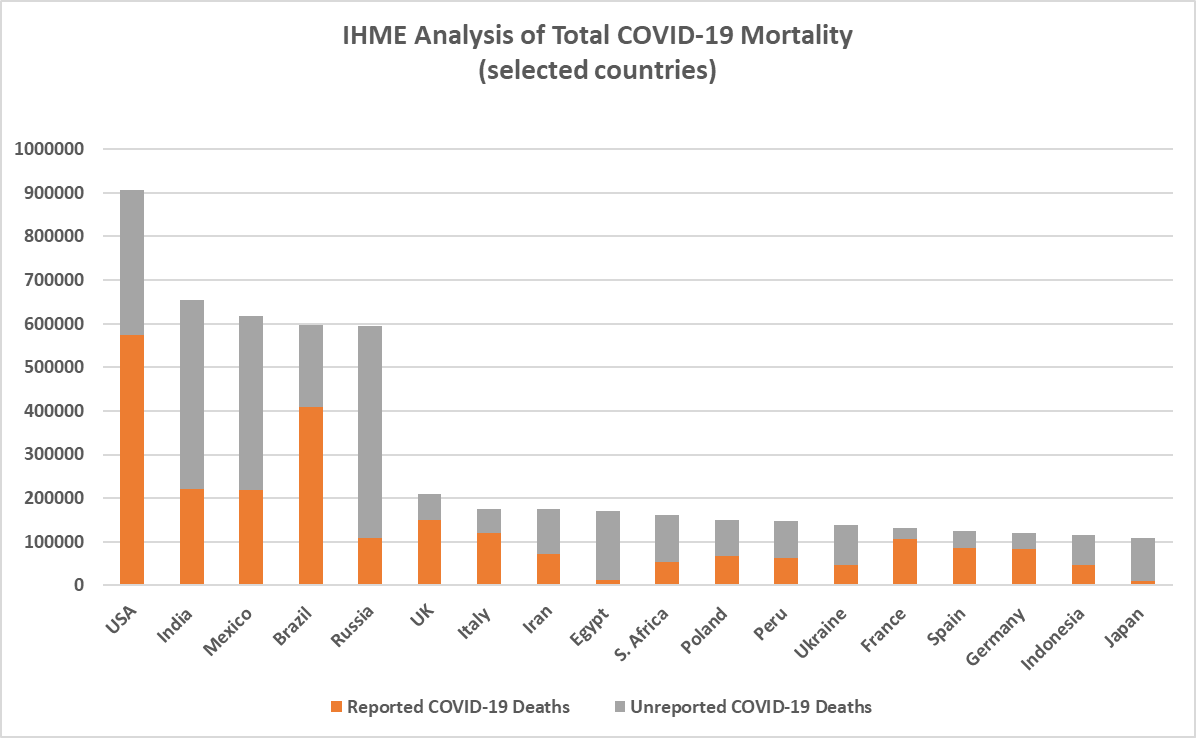
We can see that some countries have a bigger under-reporting problem than others, and that sometimes the unreported deaths dwarf the reported ones, such as in India, Mexico, Russia, Egypt and Japan. It seems that not only can direct health-care provision be overwhelmed by a pandemic, but also the national structures responsible for recording and reporting on deaths. This is another example of where all-cause mortality data proves more reliable than data purporting to categorise mortality by cause of death. For practitioners habituated to using national mortality data to inform judgements on risk, seeing how wrong we've been with some of these totals should be sobering indeed.
References:
Institute for Health Metrics and Evaluation (2021).Estimation of total mortality due to COVID-19, Publication: May 6th 2021 (IHME).


Add new comment